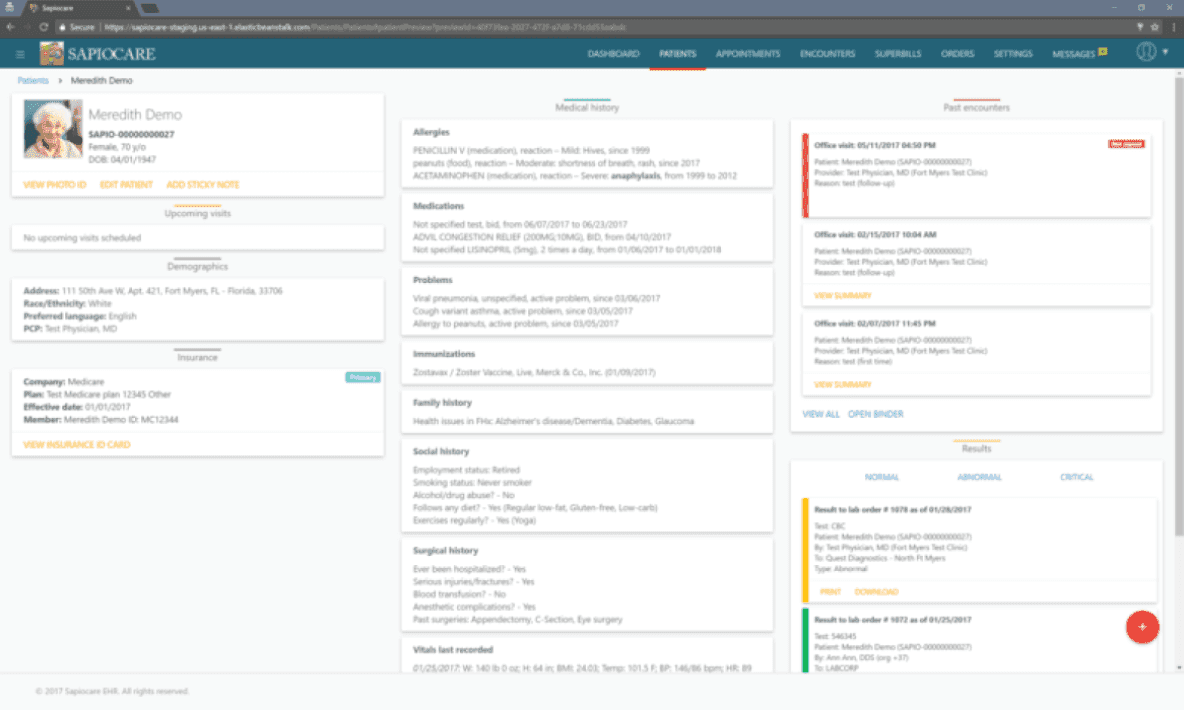
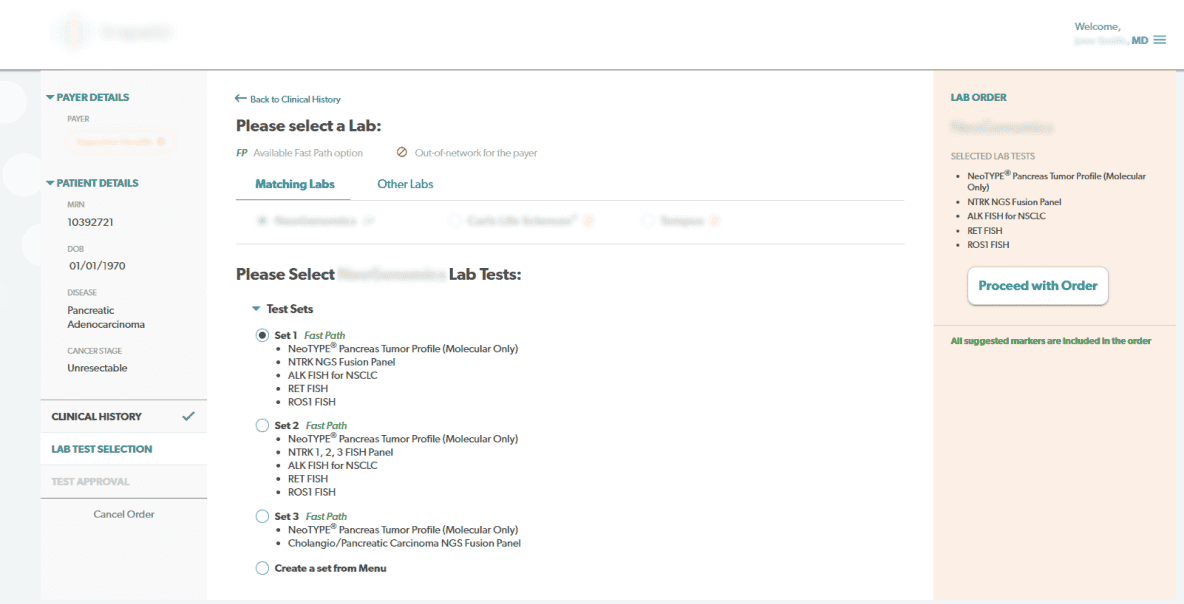
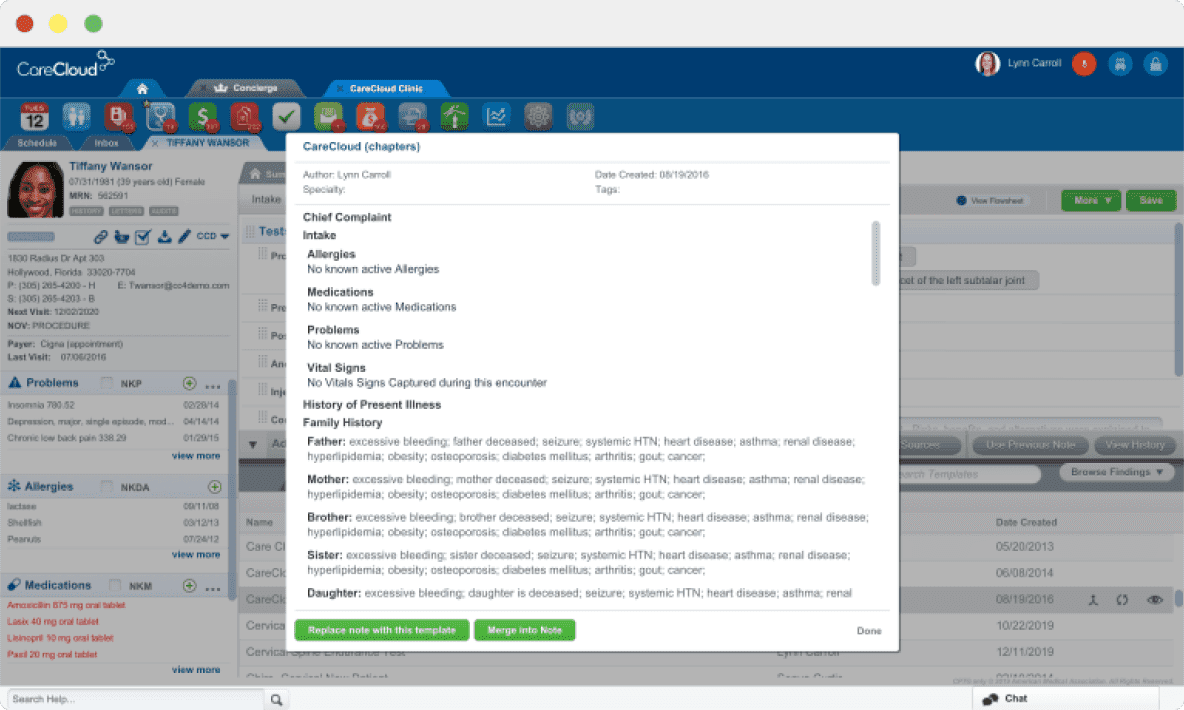
EHR vs EMR: key differences every provider should consider
April 29, 2023

Insights
EHR integration: a complete overview & real-world examples
Explore EHR integration payoffs, roadmap, and real-life examples, as well as healthcare software to integrate with EHRs to improve care quality.

Case study
A remote patient monitoring and mobile telehealth suite
Learn how Itransition developed a remote patient monitoring and telehealth platform for sexual assault victims for a US research center.

Case study
Asthma monitoring software suite
Discover the tips and tricks behind asthma monitoring software developed by Itransition’s team to help asthma patients self-manage their condition.

Insights
Dental EHR: main features, integrations & best practices
A complete guide to successful dental EHR adoption: essential features of cloud and on-premise software, benefits, and ways to avoid potential pitfalls.
Insights
Pediatric EHR: key features, benefits, and leading platforms
Discover key features and integrations of pediatric EHRs and how to choose and implement a suitable solution, overcoming possible challenges along the way.

Insights
EHR interoperability: an end-to-end guide & best practices
Learn more about electronic health records system interoperability, its benefits, standards used, challenges, and ways to improve it in your organization.
More about healthcare software services
Services
- CRM
- Data analytics
- Healthcare mobile app development
- Healthcare software development
- Hospital inventory management software
- Hospital management software
- Medical device software development
- Medical image analysis
- Patient engagement solutions
- Patient portals
- Pharmacy management software
- Remote patient monitoring
EHR
Telehealth